A full-thickness cartilage defect refers to damage or injury to the articular cartilage that lines the surface of a joint, where the cartilage is disrupted or worn through completely, exposing the underlying bone. This can occur in various joints, but it’s commonly seen in weight-bearing joints such as the knee. The articular cartilage plays a crucial role in joint function, as it provides a smooth and low-friction surface for the bones to move against each other. When a full-thickness defect occurs, it can lead to a range of symptoms and functional limitations.
Symptoms of a Full-Thickness Cartilage Defect May Include:
1. Pain
Patients often experience pain, especially during weight-bearing activities or movement of the affected joint.
2. Swelling
Swelling may occur as a result of inflammation within the joint.
3. Joint stiffness
Limited range of motion and stiffness can be present, making it difficult to perform certain activities.
4. Catching or locking
Some individuals may notice sensations of catching, locking, or popping in the joint when they move it.
5. Instability
A full-thickness cartilage defect can lead to joint instability, making the joint feel less secure and prone to giving way.
6. Reduced function
Daily activities, sports, and physical activities may become more challenging or impossible to perform due to the joint's compromised function.
7. Osteoarthritis
If left untreated, a full-thickness cartilage defect can lead to the development of osteoarthritis, a degenerative joint disease characterized by progressive joint damage.
Exploring the Causes of Full-Thickness Cartilage Defects
A full-thickness cartilage defect can be caused by various factors, and its origins can often be classified into two main categories: traumatic and non-traumatic.
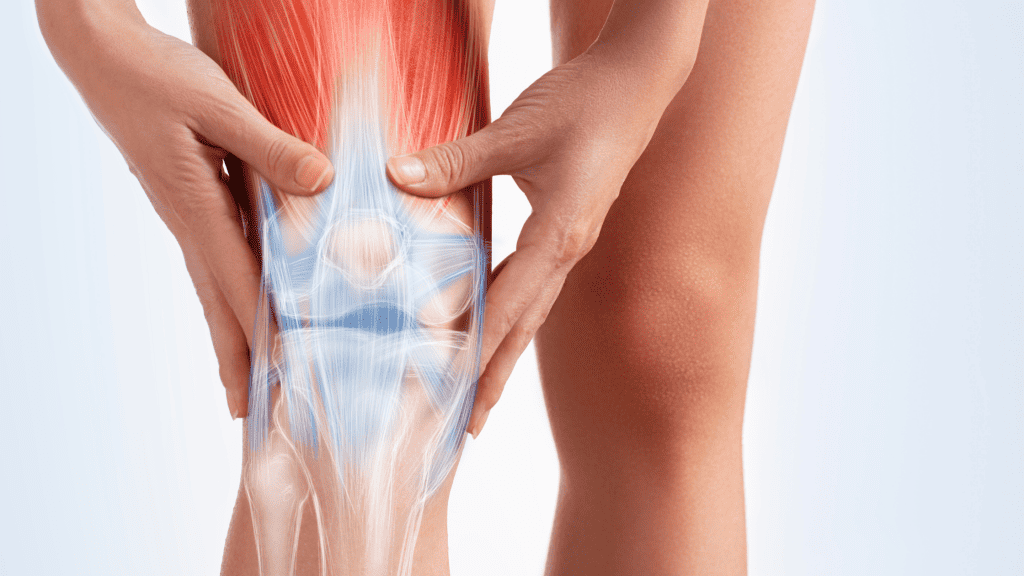
Traumatic Causes:
Injury
Sudden, traumatic injuries like sports-related incidents, falls, or accidents can directly damage the cartilage, leading to full-thickness defects.
Joint dislocation
Joint dislocation can result in cartilage damage as the bones shift out of their normal position.
Fractures
Fractures that involve the joint surface can also damage the cartilage.
Non-Traumatic Causes:
Osteoarthritis
Long-term wear and tear on the joint can result in the gradual deterioration of cartilage, eventually leading to full-thickness defects.
Age
As people age, the cartilage can naturally break down and become more susceptible to damage.
Genetics
Some individuals may be genetically predisposed to cartilage problems.
Overuse
Repetitive stress on a joint, often seen in certain occupations or sports, can contribute to cartilage damage over time.
Inflammatory conditions
Conditions like rheumatoid arthritis can cause inflammation within the joint, leading to cartilage damage.
Traditional Treatments – Non-Surgical and Surgical Interventions for Treating a Full-Thickness Cartilage Defect
Typical treatments for a full-thickness cartilage defect vary depending on the severity, location, and individual factors. Some common treatment options include:
1. Non-Surgical Options:
Physical therapy
Rehabilitation exercises can help strengthen the joint, improve its stability, and reduce pain.
Oral or topical medications
Non-steroidal anti-inflammatory drugs (NSAIDs) or pain-relieving creams may provide symptomatic relief.
Lifestyle modifications
Weight management and avoiding activities that exacerbate symptoms can be helpful.
2. Surgical Interventions
Microfracture
This is a surgical procedure where small holes are made in the exposed bone under the cartilage defect to stimulate the formation of fibrocartilage. While it can be effective for small defects, it doesn't regenerate true hyaline cartilage.
Osteochondral autograft or allograft transplantation
Healthy cartilage tissue is taken from another part of the joint or a donor and transplanted into the damaged area.
Autologous chondrocyte implantation (ACI)
A two-step procedure where a sample of the patient's healthy cartilage is cultured in a lab and then implanted into the damaged joint.
Matrix-induced autologous chondrocyte implantation (MACI)
A variation of ACI where the cultured chondrocytes are combined with a biological matrix and implanted in the joint.
Osteotomy
In some cases, realigning the bones around the joint may be necessary to shift weight-bearing and reduce stress on the damaged cartilage.
Total joint replacement
In cases of severe cartilage damage and advanced osteoarthritis, replacing the entire joint with an artificial prosthesis may be the most effective treatment.
The choice of treatment depends on the patient’s age, activity level, the size and location of the defect, and the overall health of the joint. A healthcare provider will conduct a thorough evaluation and recommend the most appropriate treatment option. It’s essential to seek medical advice to determine the best course of action for a full-thickness cartilage defect to alleviate pain, restore joint function, and prevent further joint damage.
The Next Generation Treatment for Cartilage Defects
Stem cell therapy is an emerging field with the potential to help with full-thickness cartilage defects. While it’s not a guaranteed cure, stem cell therapy has shown promise in promoting cartilage regeneration and mitigating symptoms. Here’s how it can work:
1. Stem cell sourcing
Stem cells can be obtained from various sources, such as bone marrow, adipose (fat) tissue, or blood. These cells can differentiate into various cell types, including chondrocytes, which are the cells responsible for cartilage formation and maintenance.
2. Injection into the joint
After harvesting and processing the stem cells, they can be injected into the damaged joint. The goal is to stimulate the repair and regeneration of cartilage tissue.
3. Anti-inflammatory and growth factors
Stem cells can also release anti-inflammatory and growth factors that promote healing and reduce inflammation within the joint.
4. Supporting therapies
Stem cell therapy is often used in combination with other treatments, such as physical therapy, to optimize its effectiveness.
It’s important to note that the efficacy of stem cell therapy for full-thickness cartilage defects can vary from person to person. The extent of cartilage damage, the patient’s overall health, and other factors can influence the outcomes. A patient care coordinator at GIOSTAR Chicago could help you gain a better understanding of how stem cell therapy can help your condition specifically.
Learn More About Stem Cell Therapy by Contact GIOSTAR Chicago Today
Are you suffering from a cartilage defect? GIOSTAR Chicago specializes in stem cell therapy and offers personalized stem cell therapy protocols to patients around the world. To learn more about how stem cell therapy might be able to help you, please call us or fill out the contact form and one of our patient care coordinators will reach out to you. You can also visit this page to learn more about stem cell therapy and the research behind it.
About GIOSTAR Chicago:
GIOSTAR Chicago is dedicated to developing the most advanced stem cell-based technologies and providing the best regenerative medicine for people who want to enjoy a healthy and active lifestyle.


